Opposition to antibiotics in food production is short on actual risk, but mounting pressure may lead to restrictions
It’s looking more and more like there won’t be federal legislation to restrict the use of antibiotics in food-producing animals. But that doesn’t mean pork producers are totally in the clear, says Iowa State University’s (ISU) Scott Hurd, DVM, Veterinary Diagnostic and Production Animal Medicine, College of Veterinary Medicine.
Congressional support for Preservation of Antibiotics for Medical Treatment Act, which would restrict much of the use of antibiotics in animal production, has been largely limited to the states on the east and west coasts. Hurd expects the bill will get little traction this session.
Partly in response to that legislation and to numerous other pressures, the Food and Drug Administration (FDA) has been moving steadily in recent months toward increased veterinary oversight for all uses of antibiotics, with the most concern for “production uses of medically important antibiotics,” Hurd says.
He expects FDA to set five conditions for oversight, which impacts all use of antimicrobials:
1. Evidence of effectiveness;
2. Evidence that preventive use is consistent with accepted veterinary practice;
3. Evidence that use is linked to a specific disease agent;
4. Evidence that use is appropriately targeted; and
5. Evidence that no reasonable alternatives for intervention exist.
Unlike other uses of drugs in animals (for the treatment, control and prevention of disease), the label claim for production use of antibiotics for growth promotion/feed efficiency is not directed at any identified disease or bacteria. However, that may soon change, Hurd explained in a talk at the Iowa Pork Congress in Des Moines.
“FDA’s argument is that the administration of medically important antimicrobial drugs to entire herds or flocks for non-specific purposes would represent a use that poses a qualitatively higher risk to public health than the administration of such drugs to prevent or treat illness,” he comments.
Unlike the European Union, the Food and Drug Administration in the United States is supporting the disease prevention uses of antibiotics, Hurd says.
Managing Antibiotics
Producers will need to use antibiotics “carefully and prudently” in grow-finish, follow the We Care principles outlined by the National Pork Board, and keep detailed records for FDA inspectors who may visit farms, he explains.

Consider making management changes that may reduce the need for antibiotics, including switching to an older weaning age and reducing stocking density, adds Randall Singer, DVM, University of Minnesota College of Veterinary Medicine.
Understanding Antibiotics
Singer says most people don’t understand what antibiotics are, explaining that “they are simply low molecular weight compounds that originally were produced naturally by bacteria or fungi in the environment.” What humans have done is tweak their structure so they function a little better and provide longer-lasting action.
Antibiotic approvals in the United States cover four types of uses:
1. Growth promotion/feed efficiency;
2. Disease prevention;
3. Disease control; and
4. Disease treatment.
Growth promotion or low-level use gets the most attention. The argument is that this practice doesn’t work, when in fact it does work to protect healthy animals, Singer affirms.
Disease prevention treats healthy animals that are at risk.
Use of antibiotics for disease control might be to control the spread of disease throughout the herd.
Disease treatment is the highest dose of an antibiotic given to treat a single sick animal.
When antibiotics are given to kill off bacteria, some mutate and turn resistant. The concern is that the resistant bacteria could spread from one animal to another and then onto people in the community, Singer explains.
That classic fear leads to the belief that to prevent resistant bacteria from emerging, the best solution is to give a high dose of antibiotics as quickly as possible.
“The way we are taught to use antibiotics is based on the assumption of treating tuberculosis — give the antibiotic at high doses quickly to prevent the emergence of resistance. The problem is that most of the bacteria that we are trying to kill don’t fit into the tuberculosis example,” he says.
Antibiotics don’t just target one bacterium, they affect everything in the host — including humans. “If you completely wipe out the normal bacteria, you put yourself at risk; the biggest risk for acquiring an antibiotic-resistant infection is prior use of antibiotics, not the creation of antibiotic resistance on a farm,” he observes.
“The point is we don’t want to use antibiotics in food animals at doses high enough that we completely wipe out their normal bacterial flora. Because growth promotion/feed efficiency doses do not necessarily kill the normal flora of the animal, they might help keep that animal in a healthier place,” Singer emphasizes.
Failure of Denmark’s Approach
Dogma in the literature strongly suggests giving a very high dose in short-term therapy to avoid antibiotic resistance.
“Unfortunately, that is not what the literature is actually saying today, and work in my lab and in others around the world has shown that it is those high doses that select for resistance most strongly,” Singer observes.
When critics charge that low doses of antibiotics cause resistance and cite examples such as those from Denmark, Singer says, “We should look carefully at their data.”
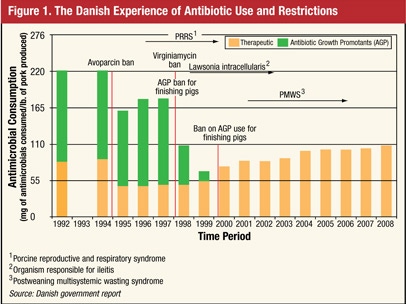
In the late 1990s, Denmark banned the routine use of several common antimicrobials in animal production due to concerns about the development of antibiotic resistance and efforts to improve human health (Figure 1). Since that time, therapeutic use of antibiotics in Denmark, many of which are the exact same products as were used in feed, continues to rise.
“The reason is that they are dealing with illnesses in pigs that were under control before the ban, and now they have to use therapeutic antibiotics to deal with problems like severe ileitis.”
Singer questions: “Would you rather keep your animals healthy in the first place, or would you rather be using important antibiotics at high doses to treat sick animals that are intended to end up in the food supply?” He says the public needs to hear this message.
Resistance vs. Risk
Antibiotic resistance is definitely cropping up more often in hospitals, and it is good to see that doctors realize they’ve been prescribing too many antibiotics — and now are trying to back away from that practice, Hurd says.
Realize there is risk in every activity, and there is no such thing as zero risk. Sound science proves there is minimal risk of human health harm from use of antibiotics based on what producers are doing on the farm, he says.
Take the recent study showing that flies at hog farms in Kansas and North Carolina carry resistant bacteria. That’s not really a big surprise. It should be a concern, but that is not saying there is any real risk, Hurd counters.
A lot of complicated connections have to be made before resistant bacteria find their way from a farm to a consumer. In this case, the bacteria carried by the flies weren’t even the kind that causes illness in humans.
So the lesson is to evaluate the level of risk that is being posed before making it more than just a concern, Hurd says. 
Antibiotic Use Reduces Carcass Contamination
During their visual inspections of pigs at slaughter, USDA food safety inspectors commonly remove clinically ill animals from the food supply. But subclinically affected pigs, with no outward signs of disease, are likely to pass inspection and may be responsible for carcass contamination and human food-borne risk, according to a study led by Scott Hurd, DVM, Iowa State University (ISU) Veterinary Diagnostic & Production Animal Medicine.
Further, the study builds on the premise that swine carcass contamination has a potential impact for human health risk from consumption of meat from carcasses contaminated with salmonella and other bacterial infections.
Hurd says other research initiatives have shown that small changes in animal health status can have large impacts on food-borne illness frequencies. Animal health management decisions on the farm — housing, antibiotic use, environment and veterinary care — can directly impact public health.
In short, “healthy pigs are less likely to be contaminated by food-borne pathogens,” Hurd stresses.
Study Premise
While sick pigs are easy to spot and remove from packing plant kill lines, pigs with underlying disease conditions that appear healthy at slaughter may have internal lesions that affect processing. Those issues may lead to cross-contamination and increased pathogen load, Hurd states in a study entitled, “Swine Health Impact on Carcass Contamination and Human Food-Borne Risk.”
Data was collected from 2,625 pigs marketed by a Midwest packing plant. In a northern Missouri operation, pigs are marketed from a single barn two or three times. The first pigs marketed are those achieving acceptable weights. Samples of the first-pull, healthiest pigs were taken first in the morning to avoid cross-contamination. Samples were then taken from other conventionally raised pigs and then antibiotic-free pigs. No differences were observed.
Identifying Risks
A total of 280 carcasses over eight replicates were swabbed in the bung (pelvic) cavity, pleural cavity and skin (pre-scald). One sponge was used for five carcasses, resulting in seven pools, except for pre-scald, where only one sponge was used.
Enterobacteria was recovered from a high percentage of pools, (81-96%), while salmonella was found in a relatively low percentage of pools (9-18%).
An experienced plant quality assurance official observed all 2,625 carcasses for health-related lesions. The most common lesion was the peel-out found on 7.1% of carcasses. Pleuritis and adhesions are likely due to respiratory disease earlier in life. Carcasses requiring a peel-out typically have portions of the lung attached to the pleura.
“These results indicate that as the percentage of subclinically ill animals increases, so does the percentage of carcasses with bacterial contamination,” Hurd says. The strongest relationships were identified between the percentage of peel-outs and campylobacter contamination in the pleural cavity and between peel-out percent and enterococcus contamination in the bung cavity.
As the percentage of peel-outs in a group increased by 1%, the pleural campylobacter contamination increased by 5%, and enterococcus contamination in the bung increased by 4.4%.
Hurd concludes there is a correlation between lesions suggestive of subclinical animal disease and human health risks as measured by carcass contamination. When diseases resolve, old lesions may remain and go undetected until evisceration.
In previous studies, 50% of abnormalities went undetected by European Commission detection methods. Poor evisceration techniques increased enterobacteria contamination from 4% to 40%. Dressing, splitting and meat inspection can account for 85% to 90% of carcass contamination.
“So lesions affecting evisceration quality will impact public health risk by increasing carcass handling and cross-contamination,” he says.
A Related Study
In a second, related study, 358 carcasses were selected from a Midwest operation of conventional- and antibiotic-free raised pigs to determine a correlation between swine carcass lesions and salmonella contamination.
Unlike the first study, when a pooled sampling method was used, in this study carcass swabs were collected from individual animals and matched with lesion data for every tested carcass.
Animals stressed or immune-compromised by long-term, low-grade illness are more likely to be shedding upon arrival at the packing plant, with food-borne pathogens, especially salmonella. Abscesses or adhesions provide means for cross-contamination at slaughter.
The positive correlation observed between salmonella contamination and lesions was compromised by the small number of samples tested, but still indicated a potential health impact across the 95 million pigs harvested per year in the United States, Hurd says.
About the Author(s)
You May Also Like




